Blog
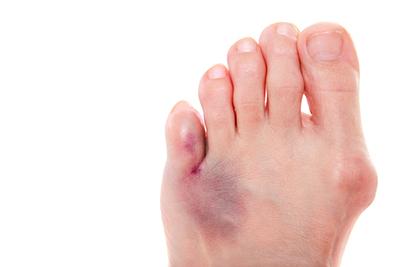
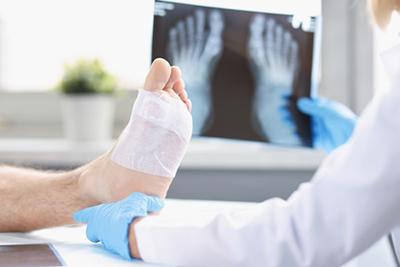
Toe Fractures: Causes and Prevention
- posted: Apr. 10, 2024
A toe fracture occurs when one of the bones in your toe breaks. Common symptoms include pain, swelling, bruising, and difficulty moving the affected toe. If you notice these signs, Read More
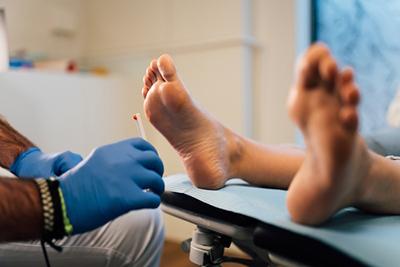
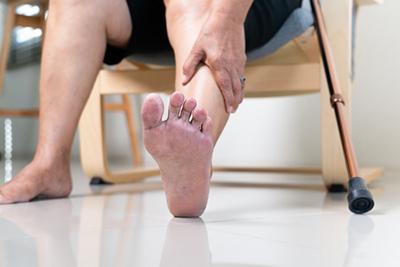
Diabetic Foot Care: Importance, Tips, and Warning Signs
- posted: Apr. 08, 2024
When you’re dealing with diabetes, you may understand that one of the most important things you can do is care for your feet. For individuals living with diabetes, proper foot Read More
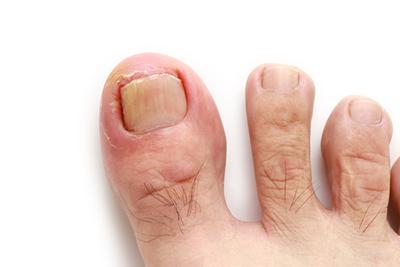
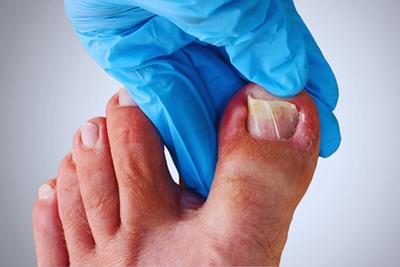
Symptoms of an Ingrown Toenail
- posted: Apr. 01, 2024
Ingrown toenails are painful and ugly. They can make it difficult to put on shoes, to stand, and to walk without pain. An ingrown toenail can decrease your mobility. Your Read More
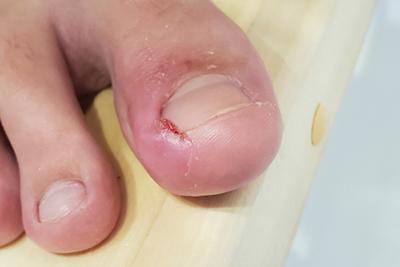
Complications of Untreated Ingrown Toenails
- posted: Mar. 20, 2024
Ingrown toenails can unexpectedly disrupt our daily lives, often arising from simple activities like improper nail trimming or wearing ill-fitting shoes. After a long day, you notice a sharp pain Read More
Treating Plantar Fasciitis
- posted: Mar. 15, 2024
If you are experiencing stabbing, aching heel pain on the side of your foot, or running across your heel, you could have a very common condition known as plantar fasciitis. Read More
Understanding Flat Feet: Causes, Symptoms, and Diagnosis
- posted: Mar. 06, 2024
Flat feet refer to a condition in which your foot’s arch collapses. According to Dr. Gary Rogers of Wilmette Foot and Ankle Clinic - which serves the North Shore, Chicago, Read More
Managing Your Heel Pain
- posted: Mar. 01, 2024
Your heels are nature’s shock absorbers, providing a cushion for standing, walking, and running. If you’ve ever experienced heel pain, you already know how it can impact your life. The Read More
When To Seek Professional Help for Ingrown Toenails
- posted: Feb. 22, 2024
Ingrown toenails are a common condition in which the corner or side of a toenail grows into the skin. The result is pain, inflamed skin, swelling, or infection. Ingrown toenails Read More
The Role of Podiatry in Managing Foot and Ankle Fractures
- posted: Feb. 09, 2024
Foot and ankle fractures are a common problem, especially as you get older. Bones become more brittle, and you are less flexible than you once were. Foot and ankle fractures Read More
What You Need To Know About Ingrown Toenails
- posted: Feb. 01, 2024
Ingrown toenails can happen to anyone. If you have an ingrown toenail, chances are it’s difficult to put on shoes and want to walk around. Your podiatrist can help with Read More
The Impact of Plantar Fasciitis on Athletes and Active Individuals
- posted: Jan. 22, 2024
When you’re active, you often spend a lot of time on your feet. This means that your feet are taking on a lot of pressure from the weight of your Read More
Sports Podiatry: Addressing Foot and Ankle Injuries in Athletes
- posted: Jan. 08, 2024
As an athlete, you know how critical it is to stay at the top of your game and remain in optimal physical shape. Your feet and ankles are the foundation Read More
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
- posted: Jan. 01, 2024
Do you have foot problems? Do your feet hurt all the time? If so, you need to discover the benefits of orthotics. This common treatment, available from your podiatrist, can Read More
Diabetic Foot Care: Preventing Complications and Maintaining Foot Health
- posted: Dec. 07, 2023
Diabetes, a condition affecting how your body uses sugar, impacts various organs, including your feet. High blood sugar can lead to nerve damage (neuropathy) and poor circulation, increasing the risk Read More
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
- posted: Dec. 01, 2023
If you experience a foot injury, it can dramatically impact your quality of life. Depending on the injury, foot injuries can lead to loss of mobility, inability to drive, lost Read More
Our Location
1919 Lake Ave Ste A
Wilmette, IL 60091-1480